Using CT Scans in Surgical Decision-Making in Peritoneal Mesothelioma
Peritoneal mesothelioma is caused by asbestos. The peritoneum is the space in your abdomen that contains the intestines, the stomach, and the liver. The abdomen (peritoneum) is the second most common site of mesothelioma after the pleural (lungs and chest).
Most doctors believe peritoneal mesothelioma is caused by the ingestion of asbestos fibers. Microscopic asbestos fibers become embedded in the abdomen (peritoneum).
After about 20-50 years, these fibers can cause inflammation and mutations in the healthy mesothelial cells. These mutations may ultimately cause these cells to become cancerous. Thus, forming tumors in the peritoneum.
Patients diagnosed with peritoneal mesothelioma may survive several or more years after diagnosis. There are long-term survivors, such as Paul Kraus.
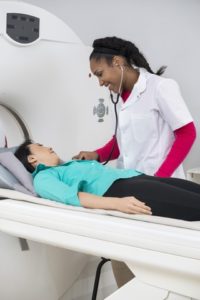
Using CT Scans to Avoid Unnecessary Surgery
We have all heard of CT or CAT scans. CT stands for computed tomography scans which is a type of X-ray. In fact, CT scans are just a more sophisticated use of X-ray technology.
Many clinicians use CT scans for surgical decision-making in peritoneal mesothelioma. In fact, CT is the first imaging choice for evaluating patients with peritoneal mesothelioma.
Results of a new study show that CT is also a good technique for identifying patients who may not benefit from surgery.
Peritoneal mesothelioma commonly presents with nonspecific symptoms such as abdominal pain. Patients with aggressive cancer types or advanced disease may not benefit from unnecessary surgery.
Understanding Peritoneal Mesothelioma
There are five cell types of peritoneal mesothelioma. This is important because each type has its own symptoms and prognosis.
The most common cell types include epithelioid, sarcomatoid, and biphasic mesothelioma. These are all highly malignant types of peritoneal mesothelioma with poor prognosis.
At first, malignant peritoneal mesothelioma was considered fatal. The introduction of cytoreductive surgery (CRS) and hyperthermic intraperitoneal chemotherapy (HIPEC) offer hope. In a few select cases, long-term survival and cure could be achieved.
Yet, the survival benefits following CRS and HIPEC depend on the complete removal of cancer cells. But removing all cancer cells can cause other side effects.
New Role of Clinical Imaging in Peritoneal Cancer
A new study released in Insights into Imaging found a new way for doctors to decide who benefits from surgery. A team of Indian clinicians looked at the role of clinical imaging in surgical decision-making in patients with peritoneal mesothelioma.
They coined a new acronym ‘PAUSE’. It stands for peritoneal cancer index, ascites and abdominal wall disease, unfavorable sites of involvement, small bowel and mesenteric disease, and extraperitoneal disease.
Yes, this is a mouthful!
But the components of ‘PAUSE’ are important when doctors are trying to decide on a treatment plan. This gives doctors a way to decide who benefits the most from these surgeries.
The goal of ‘PAUSE’ is to determine patients who might not benefit from CRS and HIPEC. Thus, avoiding unnecessary surgeries.
CT imaging has a crucial role in aiding surgical decision-making. ‘PAUSE’ focuses on key elements to determine feasibility, prognosis, and benefits from surgery. Using ‘PAUSE’ in peritoneal mesothelioma patients works.
Source
Chandramohan, Anuradha, Nehal Shah, Andrew Thrower, Norman John Carr, Rohin Mittal, Faheez Mohamed, and Brendan Moran. “Communicating imaging findings in peritoneal mesothelioma: the impact of ‘PAUSE’on surgical decision-making.” Insights into Imaging 12, no. 1 (2021): 1-18. https://link.springer.com/article/10.1186/s13244-021-01118-y