Mesothelioma Surgeon Says Proper Staging Key to Radical Surgery Survival
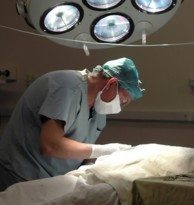 One of the country’s top mesothelioma surgeons has just published a study he says confirms the role of lymph node involvement in survival after radical mesothelioma surgery.
One of the country’s top mesothelioma surgeons has just published a study he says confirms the role of lymph node involvement in survival after radical mesothelioma surgery.
Dr. David Sugarbaker, Director of the Lung Institute at Baylor College of Medicine in Texas, is one of the most experienced practioners of a radical surgical approach to malignant pleural mesothelioma called extrapleural pneumonectomy. EPP aims to prevent the spread or return of mesothelioma by not only removing the tumor and the pleural lining on which it is located, but also the nearest lung, all or part of the diaphragm, the lining around the heart, and other at-risk tissues.
The procedure is controversial because of its high rate of complications and death. Some studies, including the MARS (Mesothelioma and Radical Surgery) trial, have suggested that the risks of EPP outweigh the benefits and some prominent doctors recommend that surgeons use the more conservative pleurectomy/decortication procedure instead.
But in a new study in the Annals of Surgery, Dr. Sugarbaker and his colleagues present evidence that survival after EPP has a lot to do with how far into the lymph system mesothelioma has spread. The team evaluated the cases of 529 patients with epithelioid pleural mesothelioma who underwent EPP between 1988 and 2011. The median age of the patients was 59 and 75% of them were men.
In the Baylor study, 5% of the mesothelioma patients who had EPP died either in the hospital or within 30 days of surgery. But 4% of patients who had the radical procedure lived for 10 years or more. Sixty-seven percent lived for at least a year after surgery and 14% were still alive at 5 years. The difference appeared to be influenced, in part, by whether or not the cancer had spread to patients’ lymph nodes.
When mesothelioma was confined to the tumor, patients lived for a median of 26 months after the procedure, whereas those with cancer in one or two of the closest sets of lymph nodes (N1 or N2) to the tumor had a median survival of just 13 to 17 months.
“This study confirms that lymph node status is significantly correlated with overall survival in patients with epithelioid malignant pleural mesothelioma undergoing EPP and suggests that those with simultaneous involvement of N1 and N2 stations are at increased risk,” concludes the study. Dr. Sugarbaker says the results underscore the need for thorough staging of pleural mesothelioma prior to surgery.
Source:
Sugarbaker, D et al, “Extrapleural Pneumonectomy in the Treatment of Epithelioid Malignant PleuralMesothelioma: Novel Prognostic Implications of Combined N1 and N2 Nodal Involvement Based on Experience in 529 Patients”, October 2014, Annals of Surgery, pp. 577-582.





