Study Confirms Feasibility and Safety of Minimally Invasive Mesothelioma Surgery
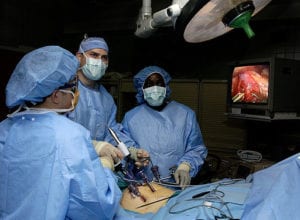 New research suggests that the future of surgery for peritoneal mesothelioma could be much less invasive than it is now—at least for select patients.
New research suggests that the future of surgery for peritoneal mesothelioma could be much less invasive than it is now—at least for select patients.
The study focused on patients with tumors that had spread to the peritoneal membrane that lines the abdomen. This is the place where malignant mesothelioma starts.
In a report published in the journal Surgical Endoscopy, an international team of experts concludes that minimally invasive surgery for peritoneal cancers like malignant mesothelioma is both feasible and safe and should be considered for certain patients.
CRS/HIPEC Standard of Care for Malignant Mesothelioma
Currently, the standard of care for peritoneal mesothelioma is cytoreductive surgery to remove as much of the tumor as possible followed by a rinse of heated chemotherapy drugs (HIPEC) to kill any residual cells. It is traditionally performed by making a long abdominal incision.
A complex multi-part procedure, CRS/HIPEC has dramatically changed the odds of surviving peritoneal mesothelioma.
But CRS/HIPEC has its drawbacks. Because it is a major open surgery, patients must be in otherwise reasonably good health to be considered candidates. It is not an option for fragile mesothelioma patients or those with multiple other health problems. The pain, recovery time, and risks of CRS/HIPEC are in line with other types of major abdominal surgery.
Minimally Invasive Surgery for Peritoneal Mesothelioma
Minimally invasive surgical techniques, using cameras and small incisions, are playing an increasingly important role in the treatment of many types of cancer.
Earlier this year, a team of surgeons at University Hospital Reina Sofia in Cordoba, Spain successfully performed minimally invasive CRS/HIPEC on eight abdominal cancer patients (including two with peritoneal mesothelioma).
This week, their experience and that of surgeons at six other centers around the world, is the subject of a retrospective study from the American Society of Peritoneal Surface Malignancies.
Future Looks Good for New Approach
After reviewing the cases of 90 peritoneal cancer patients treated with minimally invasive CRS/HIPEC, the ASPSM found that only fifteen had relapsed after two-and-a-half years and only five had developed new tumors in the same region.
“Analysis of these data suggests that minimally invasive approach for peritonectomy procedures and HIPEC is feasible, safe and should be considered as part of the armamentarium for highly selected patients with peritoneal surface malignancies,” concludes the report.
The ASPSM says a peritoneal mesothelioma patient could be a candidate for minimally invasive CRS/HIPEC if their tumor is small (a peritoneal cancer index of 10 or less).
In the study, the carefully-selected patients who underwent the less invasive procedure had complete cytoreduction. There were no surgery-related deaths and only 5 percent of patients had to be readmitted to the hospital.
Sources:
Arjona-Sanchez, A, et al, “A minimally invasive approach for peritonectomy procedures and hyperthermic intraperitoneal chemotherapy (HIPEC) in limited peritoneal carcinomatosis: The American Society of Peritoneal Surface Malignancies (ASPSM) multi-institution analysis”, July 12, 2018, Surgical Endoscopy, Epub ahead of print
Arjona-Sanchez, A, et al, “Cytoreductive Surgery and Intraperitoneal Hyperthermic Chemotherapy (HIPEC) by Minimally Invasive Approach, an Initial Experience”, April 24, 2018, World Journal of Surgery, Epub ahead of print





